
Document Permanent Cervical Ligament Injury – When MRI/CT Miss the Damage
DMX (Digital Motion X-Ray) combines weight-bearing + motion to document cervical ligament damage commonly missed by static X-ray, MRI, and CT.
Why Attorneys Use DMX to Identify Cervical Ligament Injury Missed by Traditional Imaging?
Most personal injury cases are evaluated with MRI, CT, and routine X-rays. Those studies are valuable—but they primarily document static anatomy (fracture, disc pathology, gross findings). They are not designed to test cervical ligament function or evaluate spinal stability under load and during motion.
That matters because a large portion of collision-related cervical injuries involve cervical ligament injury. Cervical ligaments control motion and contribute to spinal stability. When there is ligament damage, abnormal motion can occur during everyday movement. This abnormal motion is often a major driver of persistent symptoms and functional loss—yet it can remain undocumented when imaging is static or unloaded.
Attorneys are not doctors, and most have never been taught what cervical ligament injury is, why an MRI can miss ligament damage that affects function, or that many providers are not looking for ligament injury because their tools don’t evaluate stability during motion under load.
Digital Motion X-Ray (DMX) evaluates the cervical spine under the conditions that reveal ligament injury: weight-bearing + motion. You can’t test a joint for instability if it doesn’t move. You can’t evaluate a load-bearing structure without load. DMX combines both—so abnormal motion patterns consistent with cervical ligament damage can be seen and documented.
Ligament injuries may heal with permanent structural change and reduced ligament function. When cervical ligament damage persists, clients can experience long-term problems such as ongoing pain and activity intolerance, recurring flare-ups with normal movement, reduced function and endurance, and chronic muscle guarding and secondary symptoms.
For attorneys, DMX is valuable because it helps identify and document the real damages and total damages to the cervical spine that are commonly missed by static or unloaded studies—so the medical record more accurately reflects the true injury.
What is Digital Motion X-Ray (DMX)?
Digital Motion X-Ray (DMX) is a real-time, dynamic imaging system that allows doctors to view the cervical spine while the patient moves. DMX uses fluoroscopy (an “X-ray movie”) to capture cervical motion in real time instead of relying on one still image.
DMX is designed to evaluate cervical ligament function under real-world conditions—weight-bearing + motion—so cervical ligament injury and ligament damage can be identified and documented when static or unloaded imaging fails to reveal the true injury mechanism.
DMX is one of the few tests that evaluates cervical stability under weight-bearing + motion, helping document subtle ligament injury/laxity (“sub-failure” injury) that may not be visible on routine MRI, CT, or static X-rays.

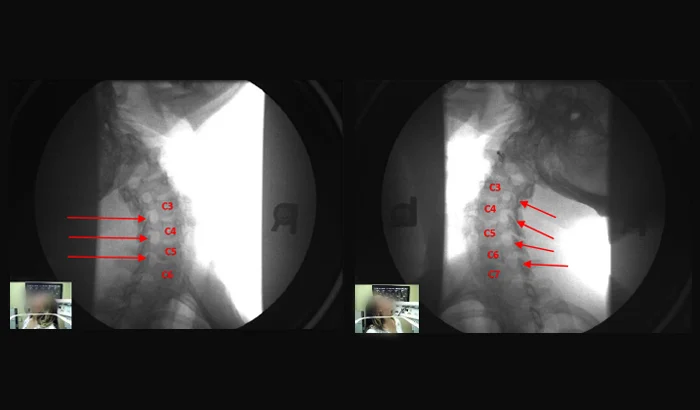
What Cervical Ligament Injury Looks Like on DMX?
When cervical ligaments are injured, they can lose normal function and the cervical joints may no longer stay stable during movement. On DMX, this can appear as excessive motion between vertebrae and joints during controlled motion under load—motion that would not be visible on a static X-ray and may not be evaluated on supine MRI/CT.
DMX captures the cervical spine in real time while the patient moves in a weight-bearing position, allowing abnormal translation/angulation patterns to be seen, reviewed, and documented—including cases where ligament injury is contributing to symptoms and functional loss..
Upper Cervical (C0–C2): An Overlooked Region Where Ligaments Matter Most
The upper cervical spine (C0–C1 and C1–C2) contains no intervertebral discs and depends heavily on ligament function for stability. This region represents a significant portion of cervical spine mechanics and is often under-evaluated when imaging workflows focus primarily on discs and static findings.
Upper cervical ligament injury can contribute to symptoms and functional loss and may be incompletely assessed without weight-bearing, motion-based evaluation.
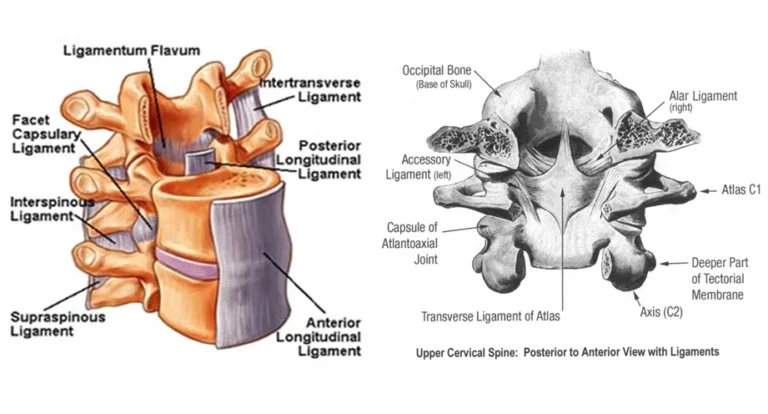
22 Key Cervical Ligaments Evaluated for Stability
Ligaments are tough connective tissues that connect bone to bone and guide normal joint motion. In the cervical spine, ligament function is essential for keeping the vertebrae stable during everyday movement and load.
Our DMX analysis evaluates 22 major cervical ligaments and related stabilizing structures for signs consistent with ligament injury and ligament damage. In practical terms, “ligament damage” can include stretching, elongation (laxity), partial tearing, and loss of normal ligament function—changes that can allow excessive motion between vertebrae and joints during movement.
The 22 major ligaments evaluated include:
- Posterior Longitudinal Ligament
- Anterior Longitudinal Ligament
- Right and Left Alar Ligaments
- Right and Left Accessory Ligaments
- Transverse Ligament
- Five Right Capsular Ligaments
- Five Left Capsular Ligaments
- Five Interspinous Ligaments
Why this matters and why it can be permanent?
Unlike a simple muscle strain, ligament injury can heal with permanent structural change and reduced ligament function. When ligaments heal with residual laxity, the result can be ongoing instability patterns, recurring flare-ups, and long-term functional limitation—especially when the neck is load-bearing and moving.
In practical terms, this can affect a client’s activities of normal life: the ability to work consistently, tolerate a full day without escalating symptoms, drive, sit at a desk, lift/carry, exercise, sleep normally, and complete routine activities of daily living without flare-ups. Many clients report that normal movements and routine demands trigger symptoms because the cervical spine is being stressed during everyday motion and load. Over time, this can contribute to reduced capacity, reduced endurance, and long-term lifestyle limitation rather than a short-term “strain” that simply resolves.
Over time, abnormal motion and chronic instability can also contribute to accelerated wear-and-tear changes, including earlier degenerative changes in cervical joints and discs. In other words, ligament damage can create a long-term mechanical problem that may progressively stress the cervical spine beyond what would be expected with normal aging.
Attorney Referral & Information Request
Objective Documentation (Mensuration / CRMA)
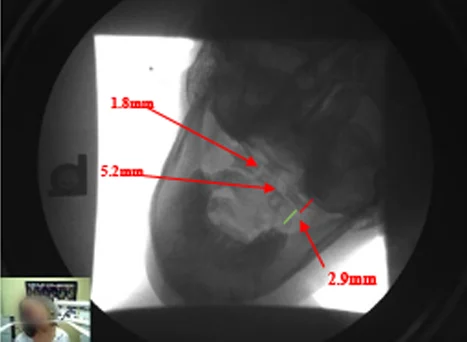
DMX motion X-rays can be analyzed using Computerized Radiographic Mensuration Analysis (CRMA) to provide objective, repeatable measurements of cervical motion. This turns a motion study into documented findings that can be reviewed, compared, and referenced rather than relying on description alone.
When appropriate, CRMA-style mensuration is used to document:
- Translation (movement between vertebrae measured in millimeters)
- Angular change (changes in alignment/angulation during motion)
- Abnormal motion patterns consistent with cervical ligament injury and instability
These objective measurements help define the extent of abnormal motion and support clearer medical documentation of ligament injury and ligament damage.
Medical Proof: AMA Guides and Permanent Impairment (Cervical AOMSI)
The AMA Guides to the Evaluation of Permanent Impairment (5th Edition, Chapter 15 — The Spine) recognize Alteration of Motion Segment Integrity (AOMSI) (also described as “loss of motion segment integrity”) as an objective basis used in permanent impairment evaluation when cervical instability is documented on motion imaging.
For attorneys, the significance is that when cervical ligament injury results in measurable instability, the medical record can move beyond a minimized “soft tissue” label toward objective documentation that treating providers may utilize when discussing permanency and, where applicable, impairment analysis under AMA Guides concepts.
Important: DMX is diagnostic imaging and does not assign impairment ratings or determine case value. Impairment and permanency opinions must be made by the appropriate licensed provider using the full clinical record and applicable guidelines.
Florida Permanent Injury Threshold (§627.737(2))
In Florida motor-vehicle cases, non-economic damages (pain and suffering) generally require meeting the statutory threshold in Fla. Stat. §627.737(2). The statute lists the following qualifying criteria:
- Significant and permanent loss of an important bodily function
- Permanent injury within a reasonable degree of medical probability (other than scarring or disfigurement)
- Significant and permanent scarring or disfigurement
- Death
For most cervical injury cases, the focus is typically on the first two criteria permanent injury and/or significant permanent loss of function and those determinations are made through medical provider opinion within a reasonable degree of medical probability, supported by objective findings.
How DMX helps support Florida permanency criteria
Traditional imaging is often static and/or unloaded, which can fail to document the true injury mechanism when the problem is cervical ligament injury and instability. DMX helps because it evaluates the cervical spine under the conditions where instability is most likely to appear: weight-bearing + motion.
DMX can provide objective documentation that treating providers may use to support permanency analysis by showing:
- Abnormal motion patterns between vertebrae/joints under load, consistent with cervical ligament injury
- Objective measurement documentation (when appropriate) to support the clinical narrative
- A clearer explanation for persistent symptoms and functional loss that are otherwise minimized as “soft tissue” when instability is not documented
Important: DMX is diagnostic imaging. It does not make the legal determination or assign case value. Permanency opinions must be rendered by the appropriate licensed provider using the full clinical record.
About the Provider
Dr. Mark N. Berry, D.C.
Diagnostic Motion X-Ray (DMX)
Dr. Berry provides DMX diagnostic imaging focused on weight-bearing, motion-based evaluation of the cervical spine. His work emphasizes objective documentation of cervical ligament injury, abnormal motion patterns, and cervical stability findings to support clear clinical reporting for personal injury cases.

Attorney FAQ
What is DMX?
DMX is weight-bearing, motion-based fluoroscopic imaging of the cervical spine. It records cervical movement in real time while the spine is under functional load.
How is DMX performed?
DMX is typically performed with the patient standing (loaded) while the neck is guided through controlled motion. The study captures the vertebrae moving during motion, rather than a single static image.
Why can cervical ligament injury be missed on MRI, CT, and routine X-rays?
Cervical ligament injury often affects ligament function and spinal stability. Static or unloaded studies are not designed to test how the cervical spine performs during motion under load.
Why is motion essential?
You cannot test a joint for instability if it does not move. Ligament injury affects how motion is controlled.
Why is weight-bearing essential?
The spine is load-bearing. Evaluating the cervical spine without load may miss functional instability that shows up under real-world conditions.
Is DMX only useful when MRI is “normal”?
DMX can be useful regardless of MRI findings because it evaluates a different question: cervical stability and ligament function during motion under load.
How are findings documented?
Through motion imaging review and, when applicable, objective measurement of abnormal motion patterns (mensuration/CRMA).
Does DMX determine impairment, case value, or legal outcome?
DMX does not assign impairment ratings, determine damages, or decide legal outcomes. DMX is diagnostic imaging. However, DMX can objectively identify and document cervical ligament injury and abnormal motion patterns under load. Those findings may be utilized by the treating provider when forming opinions regarding permanency and, where applicable, impairment analysis. Attorneys may then apply the medical findings within the legal framework of the case.
How does an attorney refer a case?
Use the “Request Attorney Information” form for referral protocols, scheduling, and sample report formats.